The recent uptick in ketamine clinic and management service organization (“MSO”) clients at our law firm is pretty significant. It’s understandable given the groundswell of momentum behind state and local legalization and decriminalization of certain other psychedelics. Many companies that are exploring psychedelic medicines are making their way into the ketmaine space. Unlike psilocybin though (and definitely unlike cannabis), ketamine stands alone as a Schedule III controlled substance, and its use for the treatment of mental health disorders is “off-label”, all of which makes it hugely regulated by state and federal healthcare laws.
An interesting curveball related to the off-label treatment of patients with ketamine is the incorporation of telehealth. Telehealth is its own quasi-emerging beast in the healthcare legal world, though it’s been around for a while now. In any event, with the advent of COVID-19 and the institution of state and federal emergency orders, certain restrictions around the use of telehealth, generally, have been relaxed. More wildly, the online prescribing of controlled substances is also looser because of COVID federal emergency orders. In turn, physicians prescribing ketamine to patients are also now starting to use telehealth more and more to do so, which makes for an incredibly sticky legal situation.
Given that I’m located and licensed in California, I’m going to use it as an example for the issues that arise when telehealth combines with ketamine. In California, telehealth is defined as:
“[T]he mode of delivering health care services and public health via information and communication technologies to facilitate the diagnosis, consultation, treatment, education, care management, and self-management of a patient’s health care while the patient is at the originating site and the health care provider is at a distant site. Telehealth facilitates patient self-management and caregiver support for patients and includes synchronous interactions and asynchronous store and forward transfers.”
There are no legal prohibitions on using telehealth technology in the practice of medicine so long as the practice is undertaken by a California licensed physician who complies with state and federal privacy laws. Physicians are held to the same standard of care and retain the same responsibilities of providing informed consent, ensuring the privacy of medical information, and any other duties associated with practicing medicine regardless of whether they are practicing via telehealth or face-to-face, in-person visits.
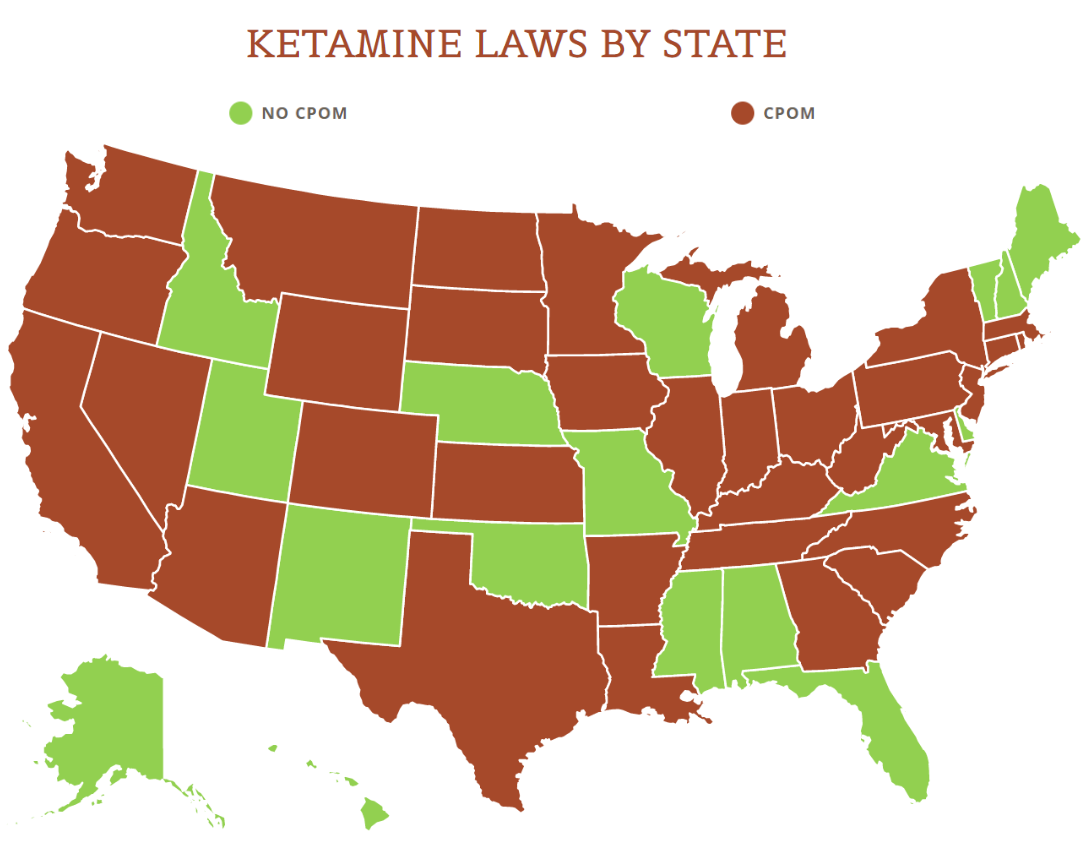
View the US Map of Ketamine Legality
Physicians using telehealth are required to establish a physician-patient relationship. The minimum requirement is to utilize a face-to-face examination if a face-to-face encounter would otherwise be required for the same healthcare service not delivered by telehealth. Unofficially, the Medical Board of California also allows a prior examination to be conducted through telehealth if the technology is sufficient to provide the same information as if the exam had been performed face-to-face.
Further, in California:
“[p]rescribing, dispensing, or furnishing dangerous drugs . . . without an appropriate prior examination and a medical indication, constitutes unprofessional conduct.” Nonetheless, “an appropriate prior examination does not require a synchronous interaction between the patient and the [physician] and can be achieved through the use of telehealth, including, but not limited to, a self-screening tool or a questionnaire, provided that the [physician] complies with the appropriate standard of care.”
Specifically regarding internet prescribing in California:
“essential components of proper prescribing include performing and documenting a physical examination that includes obtaining a legitimate medical history, engaging in sufficient dialogue to form a treatment opinion, determining the risks and benefits of the drug or treatment regimen, scheduling follow-up appointments to assess therapeutic outcome and maintaining an adequate and accurate medical record before prescribing any medication for the first time.”
Ketamine is a “dangerous drug” under California law. And even though an in-person examination is not necessarily required to conform with California telehealth laws when prescribing controlled substances, a “prior examination” is obviously still required before physicians can both engage in telehealth and prescribe controlled substances, including ketamine.
In 2018, Congress passed the Ryan Haight Online Pharmacy Consumer Protection Act of 2008 (“Ryan Haight Act”) because of “the increasing use of prescription controlled substances by adolescents and others for non-medical purposes, which [had] been exacerbated by drug trafficking on the internet.” The Ryan Haight Act is intended to prevent illegal drug activity over the Internet. The statute imposes several limitations on prescribing and dispensing controlled substances, including the directive that, with very limited exceptions, physicians can’t prescribe controlled substances over the internet without having conducted at least one in-person medical evaluation.
On April 6, 2009, the DEA published an interim final rule that, among other things, directed the DEA to create a designated registration for telehealth for the prescription of controlled substances, and subsequent laws established a one-year deadline for the DEA to set up that registration.
On September 30, 2020, the DEA published the final rule titled “Implementation of the Ryan Haight Online Pharmacy Consumer Protection Act of 2008” and adopted the interim final rule as final(the “Final Rule”), which went into effect on October 30, 2020. To date, frustratingly, there is still no regulation actually implementing the designated registration for telehealth providers.
On January 21, 2020, the declaration of a Public Health Emergency (“Order”) in response to COVID-19 temporarily allows the expanded use of telehealth in prescribing controlled substances for the duration of the Order. Specifically, the Department of Health and Human Services (“HHS”) permits DEA registrants to prescribe controlled substances without a prior in-person medical evaluation provided:
“The practitioner is acting in the usual course of his/her professional practice and the prescription is issued for a legitimate medical purpose; The telehealth communication is conducted using an audio-visual, real-time, two-way interactive communication system; and The practitioner is acting in accordance with applicable federal and state law.”
However, this exemption will expire at the end of the Order (the Order was last renewed by HHS on April 15, 2021 and no deadline for its termination has been set yet). On March 31, 2020, the DEA published “How to Prescribe Controlled Substances to Patients During the COVID-19 Public Health Emergency” that provides guidance for providers prescribing controlled substances via telehealth until the end of the Order.
Physician professional corporations (PCs) and the MSOs that serve them (especially in strict CPOM states) are starting to take advantage of the Order by interpreting it extremely liberally in order to prescribe ketamine to patients via telehealth without prior physical exams and/or just through asynchronous interactions. Given how murky the Order is and its touch-and-go nature, certain PCs, MSOs, and telehealth service providers are really pushing the buck when it comes to the precarious online prescribing of controlled substances.
Once the Order is over, many of these companies will probably see strict enforcement of the Ryan Haight Act by the DEA (unless and until the telehealth registration is actually created and implemented). Any telehealth venture that’s contemplating allowing physicians to engage in ketamine off label prescriptions and treatments really needs to do its homework about internet prescribing during and after COVID when the Order is lifted.